Answer Summary
AI-driven analytics streamline accounts receivable by shifting from reactive, manual follow-up to a predictive model that prioritizes claims based on their likelihood of resolution and financial impact. As payer automation accelerates in 2026, DME providers using AI-enabled workflows are projected to reduce Days Sales Outstanding (DSO) by 25% by identifying and resolving high-risk claims before they age into delinquency. This strategic shift transforms A/R into a proactive intelligence function, ensuring stable cash flow and significantly lowering the administrative cost per claim processed.
Introduction: Why Accounts Receivable Became the Weakest Link in the Revenue Cycle
For many DME providers, accounts receivable has historically been treated as a necessary but secondary function—important, but largely mechanical. Claims were submitted, payments arrived, and staff followed up when balances aged beyond expectations. As long as revenue totals looked healthy, A/R volatility was tolerated as part of the business.
By 2026, that tolerance disappeared.
Reimbursement delays lengthened, payer behavior became less predictable, and denial activity increased. Providers discovered that strong billed revenue did not translate into usable cash when A/R workflows lacked prioritization, visibility, and control. Traditional follow-up models—built on aging buckets and manual effort—failed to keep pace with the complexity of modern payer systems.
In this environment, A/R is no longer just about collection. It is about intelligence. Providers that leverage AI to understand risk, predict outcomes, and direct human effort strategically are moving from constant firefighting to predictable cash flow.
How Accounts Receivable Actually Breaks Down in DME Operations
To improve A/R performance, providers must first understand where it breaks down.
The A/R lifecycle typically follows a familiar path:
- Claim submission
- Payer adjudication
- Payment, denial, or delay
- Follow-up and resolution
On paper, this appears linear. In practice, it is fragmented. Visibility is often lost once a claim leaves the billing system. Staff work queues fill with mixed-priority accounts, and follow-up activity is driven by aging rather than likelihood of resolution.
Common breakdowns include:
- Claims with missing documentation that linger without clear next steps
- Delays caused by payer reviews that are mistaken for inaction
- Repeated follow-up on low-probability claims while high-risk claims stall
These breakdowns consume staff time without improving outcomes. The result is high effort with diminishing returns.
Why Manual A/R Follow-Up Fails at Scale
Traditional A/R models assume that persistence solves most problems. Staff are assigned queues, claims are worked based on age, and follow-up continues until payment or write-off.
This approach fails at scale for several reasons:
- All claims receive similar attention regardless of risk
- Staff effort is not aligned to payer behavior
- Follow-up timing is reactive, not strategic
- Burnout increases while recovery rates stagnate
As payer automation accelerates, repeated manual outreach often has little effect. Without insight into why a claim is stalled, effort is wasted.
AI changes this dynamic by introducing prioritization and prediction into A/R workflows.
What AI Actually Does in Accounts Receivable
AI in A/R is frequently misunderstood. It is not simply faster reporting or automated reminders. Its value lies in pattern recognition and prediction.
AI systems analyze historical claim outcomes to identify:
- Payer-specific response patterns
- Common causes of delay or denial
- Timing trends for payment resolution
- Attributes correlated with successful recovery
By learning from outcomes, AI provides insight that static reports cannot. This allows providers to move from reactive follow-up to anticipatory action.
Prioritization: Focusing Human Effort Where It Matters
One of the most immediate benefits of AI in A/R is intelligent prioritization.
Instead of working claims strictly by age, AI-enabled systems segment accounts based on:
- Likelihood of payment
- Risk of denial or recoupment
- Expected time to resolution
- Financial impact
High-risk, high-value claims receive immediate attention. Low-probability accounts are deprioritized or resolved through alternative paths. This targeted approach reduces wasted effort and improves recovery efficiency.
Human expertise is applied where it has the greatest impact.
Predictive Payment Timing and Cash-Flow Visibility
A/R performance is often evaluated using averages—average days in A/R, average payment time, average recovery rate. In volatile environments, averages obscure reality.
AI-driven forecasting focuses on timing distributions, not single-point estimates. By predicting when payments are likely to arrive based on payer behavior and claim attributes, providers gain:
- More accurate cash-flow forecasts
- Better purchasing and staffing decisions
- Earlier identification of liquidity risk
This level of visibility allows leadership to plan proactively rather than react under pressure.
Denial Prevention as an A/R Strategy
Many providers treat denial management as separate from A/R management. In practice, they are tightly connected.
AI enables feedback loops that connect denial data back to A/R prioritization. Claims with attributes similar to recently denied cases can be flagged early. Follow-up strategies can be adjusted before claims age unnecessarily.
By integrating denial intelligence into A/R workflows, providers reduce downstream drag and improve overall cycle performance.
Automation With Governance: Avoiding the “Black Box”
Automation without oversight introduces risk. AI-driven A/R systems must operate within clearly defined governance frameworks.
Providers should define:
- Which actions automation can perform independently
- When human intervention is required
- How exceptions are escalated
- How outcomes are reviewed and refined
Under 42 CFR § 424.57, suppliers remain accountable for billing accuracy and documentation regardless of automation. Governance ensures AI enhances control rather than obscuring responsibility.
Measuring A/R Performance the Right Way
Days in A/R remains a useful metric, but it is insufficient on its own.
Providers should also monitor:
- Resolution velocity by payer
- Recovery probability by claim type
- Staff effort per resolved account
- Percentage of A/R requiring escalation
These metrics reflect whether A/R workflows are controlled, not just busy.
Financial Impact of AI-Driven A/R Management
When implemented correctly, AI-driven A/R management delivers measurable financial benefits:
- Reduced staff rework and overtime
- Faster cash realization
- Lower appeal dependence
- Improved forecasting confidence
The greatest value comes from predictability. Stable cash flow allows providers to make strategic decisions with confidence rather than operating defensively.
Common Failure Modes When Applying AI to A/R
Providers encounter problems when they:
- Automate poor-quality data
- Ignore payer-specific nuances
- Treat AI as a replacement for expertise
- Fail to monitor and refine models
AI amplifies existing conditions. Clean data, disciplined workflows, and ongoing oversight are prerequisites for success.
How Wonder Worth Solutions Helps Providers Regain A/R Control
Wonder Worth Solutions helps DME providers assess A/R workflow maturity, evaluate AI readiness, and design governance models that align automation with compliance and operational goals. The focus is not automation for its own sake, but predictable, defensible performance.
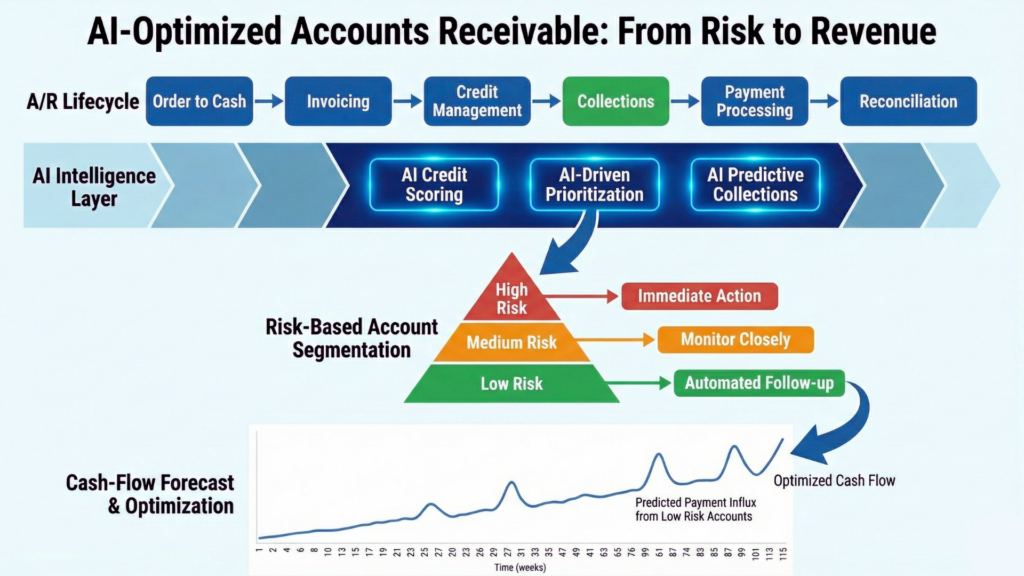
Conclusion: A/R Stability Is an Intelligence Advantage
In 2026, accounts receivable performance separates reactive organizations from resilient ones. AI enables providers to understand risk, predict outcomes, and direct effort strategically. When A/R is treated as an intelligence function rather than a collection task, cash flow becomes more predictable and operations more stable.



