Introduction:
The DME industry is dynamic, with providers facing constant challenges, from regulatory shifts to evolving patient needs. Resilient DME practice—the ability to adapt and thrive in the face of adversity—is essential for long-term success.
This blog explores how DME providers can build resilience by embracing innovation, optimizing workflows, and fostering a culture of adaptability, ensuring they stay competitive in an ever-changing landscape.
What Does Resilience Mean for DME Providers?
Resilience in the DME context means the ability to:
- Adapt to Changes: Stay flexible in response to regulatory updates, market shifts, or patient demands.
- Mitigate Risks: Identify and address vulnerabilities proactively.
- Sustain Growth: Maintain profitability and quality of care, even during challenges.
By prioritizing resilience, DME providers can safeguard their operations and position themselves for future success.
Key Strategies for Building a Resilient DME Practice
1. Embrace Automation and Technology
- Why It Matters: Automation reduces reliance on manual processes, streamlines workflows, and minimizes errors.
- How to Implement:
- Automate claims processing to reduce denial rates and improve cash flow.
- Use inventory management software to prevent overstocking or shortages.
- Impact: Enhances efficiency and ensures continuity during staff shortages or unexpected demand.
2. Diversify Revenue Streams
- Why It Matters: Dependence on a single revenue source increases vulnerability to market fluctuations.
- How to Implement:
- Offer ancillary services, such as equipment maintenance or patient education programs.
- Expand into niche markets, like pediatric or bariatric DME.
- Impact: Provides stability and cushions the practice against unexpected downturns.
3. Monitor and Mitigate Risks
- Why It Matters: Proactive risk management prevents disruptions and protects profitability.
- How to Implement:
- Conduct regular audits of workflows and compliance processes.
- Use analytics tools to identify trends and potential vulnerabilities.
- Impact: Minimizes financial and operational risks, ensuring smoother operations.
4. Invest in Staff Training and Retention
- Why It Matters: A skilled, motivated workforce is critical for adapting to change and maintaining high-quality service.
- How to Implement:
- Provide ongoing training on compliance, new technologies, and best practices.
- Foster a positive workplace culture with competitive benefits and recognition programs.
- Impact: Reduces turnover and builds a team that is equipped to handle challenges.
5. Leverage Data to Drive Decisions
- Why It Matters: Data-driven insights enable providers to identify opportunities and make informed decisions.
- How to Implement:
- Track KPIs, such as claim denial rates, patient retention, and operational costs.
- Use dashboards to monitor performance and adjust strategies in real time.
- Impact: Ensures agility and responsiveness in an evolving market.
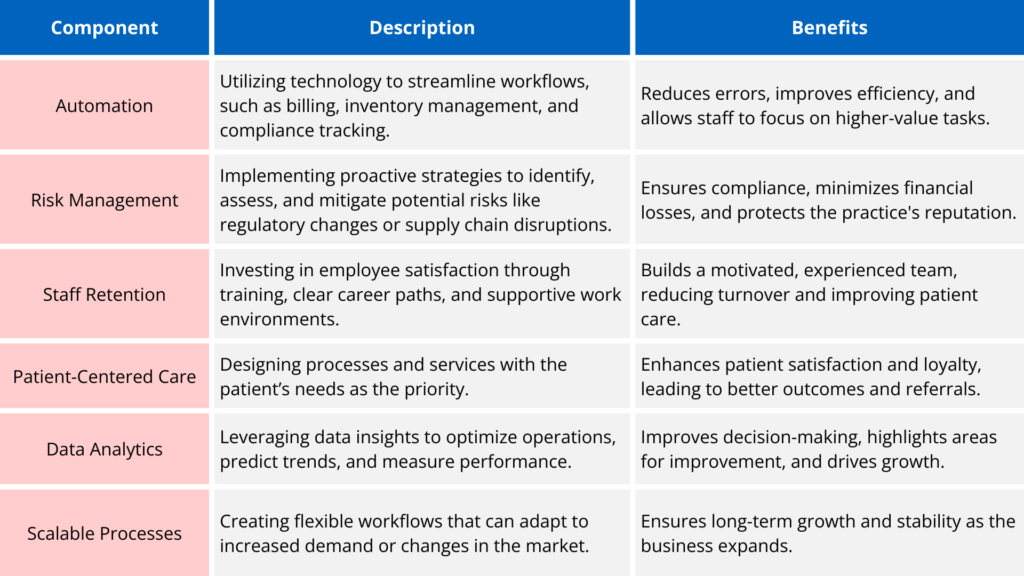
Real-World Benefits of Building a Resilient Practice
DME providers who prioritize resilience see measurable results, including:
- 20% Faster Adaptation to Industry Changes: Proactive planning reduces the impact of new regulations or market shifts.
- 30% Reduction in Operational Risks: Automation and risk management tools prevent disruptions.
- 25% Increase in Staff Retention Rates: Training and engagement foster loyalty and stability.
WWS Value Proposition
At WWS, we help DME providers build resilience with:
- Automation Solutions: Streamline workflows and reduce operational vulnerabilities.
- Analytics Platforms: Monitor performance metrics and identify areas for improvement.
- Training Programs: Equip staff with the skills to adapt to new challenges and opportunities.
Partner with WWS to future-proof your practice and ensure long-term success.



