Answer Summary
DME providers leverage telehealth to cut operational costs by compressing intake cycles and utilizing virtual assessments to capture high-quality documentation at the point of care. As virtual care is projected to represent up to 30% of all medical visits by 2026, integrating these tools allows providers to significantly reduce no-show rates and administrative rework. By shifting to a “virtual-first” infrastructure for routine follow-ups, organizations can lower overhead while maintaining the strict documentation standards required for CMS compliance.
Introduction: Telehealth Has Moved From Experiment to Infrastructure
For many DME providers, telehealth entered operations as a temporary response to access challenges. By 2026, it has become something more permanent—and more strategic.
Telehealth is no longer just about convenience. When implemented intentionally, it reduces operational friction, shortens care cycles, improves documentation quality, and lowers administrative cost. When implemented poorly, it adds complexity, frustrates patients, and creates compliance risk.
The difference is not the technology. It is how telehealth is integrated into existing workflows.
This rapid solver focuses on five practical, immediately actionable ways DME providers are using telehealth to reduce costs while improving the patient experience.
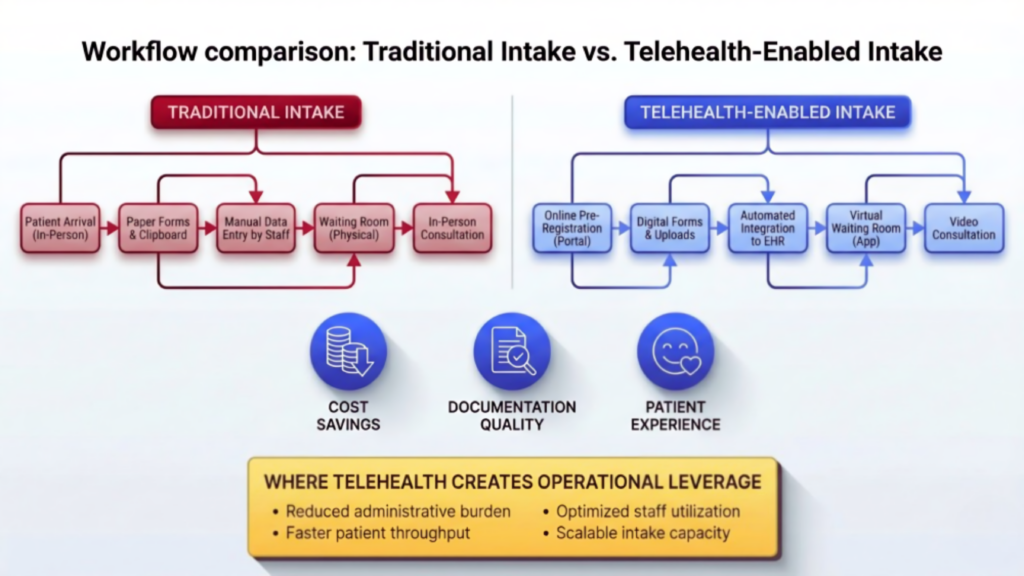
1. Reducing Intake and Qualification Costs Through Virtual Assessments
One of the most expensive stages of the DME workflow is intake qualification. Phone tag with patients, incomplete information, and repeated follow-ups consume staff time and delay care.
Telehealth enables:
- Virtual patient assessments to confirm eligibility and equipment needs
- Real-time clarification of documentation requirements
- Faster identification of missing information
Instead of multiple calls spread over days, intake teams can complete qualification in a single virtual interaction. This reduces staff touchpoints and shortens time to delivery.
The cost savings come not from replacing staff, but from compressing workflows.
2. Lowering No-Show Rates and Rescheduled Visits
Missed appointments are a hidden cost driver for DME providers. No-shows delay delivery, disrupt schedules, and create documentation gaps that surface later in billing.
Telehealth improves attendance by:
- Eliminating travel barriers
- Allowing flexible scheduling windows
- Enabling same-day virtual follow-ups
Providers that shifted follow-up visits to virtual formats consistently report lower no-show rates and faster care progression. Fewer missed interactions translate directly into smoother downstream billing.
3. Improving Documentation Quality at the Point of Care
Documentation deficiencies remain a leading cause of denials and audits. Telehealth interactions provide an opportunity to improve documentation quality in real time.
During virtual visits, providers can:
- Verify patient information live
- Confirm medical necessity details
- Capture supporting notes immediately
This reduces reliance on retrospective documentation cleanup, which is both time-consuming and risky. Stronger documentation at the point of interaction improves defensibility under 42 CFR § 424.57, which requires suppliers to maintain records supporting services billed.
4. Reducing Follow-Up and Support Call Volume
A significant portion of inbound calls to DME providers involve routine questions: equipment use, delivery status, or next steps.
Telehealth can proactively address these needs by:
- Offering scheduled virtual check-ins
- Providing visual guidance for equipment use
- Resolving questions before they escalate into repeated calls
By shifting reactive support into structured virtual interactions, providers reduce call-center volume while improving patient satisfaction.
5. Accelerating Care Cycles Without Sacrificing Compliance
Speed often comes at the expense of compliance when workflows are rushed. Telehealth allows providers to accelerate care cycles without bypassing controls.
Virtual touchpoints enable:
- Faster qualification and education
- Quicker documentation completion
- More predictable delivery scheduling
When integrated correctly, telehealth supports both efficiency and compliance rather than forcing a trade-off between them.
Where Telehealth Often Fails in DME Operations
Despite its benefits, telehealth introduces risk when poorly implemented.
Common failure points include:
- Treating telehealth as a standalone tool
- Failing to integrate virtual visits into documentation workflows
- Lack of clarity around staff roles and escalation
- Inconsistent patient communication
Telehealth should reinforce existing workflows, not operate parallel to them.
Governance and Compliance Considerations
Telehealth does not change regulatory responsibility. Documentation, medical necessity, and billing requirements still apply.
Providers must ensure:
- Telehealth interactions are documented consistently
- Records are stored securely and retrievable
- Staff understand what can and cannot be addressed virtually
Compliance discipline must extend into virtual environments.
Measuring the Impact of Telehealth Adoption
To ensure telehealth delivers value, providers should track:
- Intake cycle time
- No-show rates
- Documentation rework frequency
- Patient satisfaction feedback
- Staff time spent per case
These metrics reveal whether telehealth is improving operations or simply shifting work elsewhere.
How Wonder Worth Solutions Helps
Wonder Worth Solutions helps DME providers integrate telehealth into revenue-cycle workflows without introducing compliance or operational risk. By aligning virtual interactions with documentation standards and billing processes, providers can realize cost savings while improving patient experience.
Conclusion
In 2026, telehealth is no longer optional—but success depends on execution. DME providers that use telehealth to compress workflows, strengthen documentation, and reduce friction see measurable cost and experience benefits. Those that deploy it without structure add complexity instead of value.
Telehealth works best when it is treated as infrastructure, not an add-on.



