Introduction:
In the DME industry, success isn’t just about providing equipment—it’s about delivering quality care, maintaining efficiency, and driving profitability. Tracking key metrics (or KPIs) helps providers measure progress, identify areas for improvement, and make data-driven decisions that align with their goals.
This blog highlights the 10 most important metrics DME providers should monitor to optimize their operations and achieve long-term growth.
Why Metrics Matter for DME Providers
- Improve Decision-Making: Metrics provide objective data to guide strategies and investments.
- Enhance Operational Efficiency: Tracking performance helps identify and resolve bottlenecks.
- Boost Patient Satisfaction: Monitoring patient-focused metrics ensures high-quality care and better outcomes.
- Drive Profitability: Financial KPIs highlight revenue opportunities and cost-saving measures.
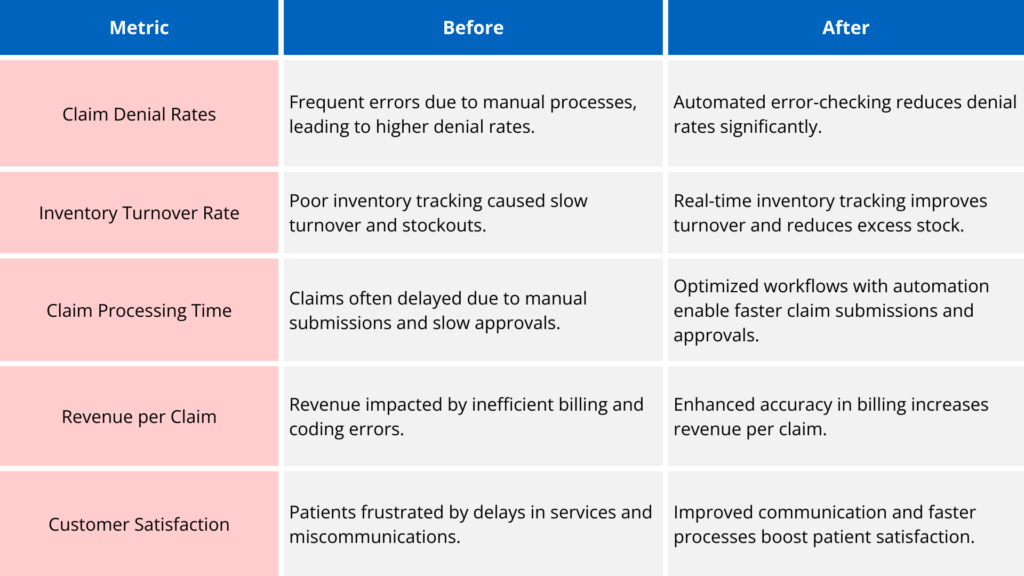
Top 10 Metrics Every DME Provider Should Track
1. Claim Denial Rate
- What It Measures: Percentage of claims denied by payers.
- Why It Matters: High denial rates indicate errors in claims submissions or incomplete documentation.
- Goal: Keep denial rates below 5%.
- Action Tip: Use automated claims validation tools to minimize errors.
2. Revenue Cycle Time
- What It Measures: Average time to receive reimbursement after submitting a claim.
- Why It Matters: Faster reimbursements improve cash flow and operational stability.
- Goal: Reduce cycle times to under 30 days.
- Action Tip: Track payer-specific timelines and follow up on delays promptly.
3. Patient Retention Rate
- What It Measures: Percentage of patients who continue using your services over a specified period.
- Why It Matters: Retaining patients is more cost-effective than acquiring new ones.
- Goal: Aim for a retention rate above 85%.
- Action Tip: Focus on patient engagement and satisfaction to build loyalty.
4. Equipment Utilization Rate
- What It Measures: Frequency and consistency of equipment use by patients.
- Why It Matters: High utilization rates reflect better adherence to care plans and improved outcomes.
- Goal: Maintain utilization rates of 90% or higher.
- Action Tip: Provide clear instructions and follow-up support to ensure correct equipment usage.
5. Inventory Turnover Ratio
- What It Measures: How often inventory is sold or used in a given period.
- Why It Matters: Optimized inventory levels reduce carrying costs and prevent shortages.
- Goal: Achieve a turnover ratio that balances stock availability and operational efficiency.
- Action Tip: Use demand forecasting tools to streamline inventory management.
6. Patient Satisfaction Score
- What It Measures: Patient feedback on their overall experience with your services.
- Why It Matters: Satisfied patients are more likely to recommend your practice and remain loyal.
- Goal: Maintain satisfaction scores of 90% or higher.
- Action Tip: Conduct regular surveys and address negative feedback promptly.
7. Cost Per Claim Processed
- What It Measures: Average administrative cost of processing a single claim.
- Why It Matters: Lower costs indicate greater efficiency in your billing and claims workflows.
- Goal: Minimize costs while maintaining accuracy and compliance.
- Action Tip: Automate claims processes to reduce manual errors and administrative time.
8. Employee Productivity Rate
- What It Measures: Tasks or claims processed per staff member within a specific timeframe.
- Why It Matters: High productivity rates reflect efficient workflows and well-utilized staff resources.
- Goal: Optimize productivity to balance workload and prevent burnout.
- Action Tip: Streamline repetitive tasks to free up staff for higher-value activities.
9. Referral Conversion Rate
- What It Measures: Percentage of referrals that convert into active patients.
- Why It Matters: Reflects the effectiveness of your referral management processes.
- Goal: Aim for conversion rates above 50%.
- Action Tip: Simplify onboarding for referred patients to ensure a smooth transition.
10. Compliance Rate
- What It Measures: Percentage of patients adhering to their care plans.
- Why It Matters: High compliance rates lead to better outcomes and lower complication rates.
- Goal: Strive for compliance rates of 85% or higher.
- Action Tip: Use automated reminders and educational tools to support adherence.
How to Start Tracking These Metrics
- Invest in Analytics Tools: Use software that integrates with your patient portals, billing systems, and inventory management platforms.
- Define Goals for Each Metric: Establish benchmarks to measure progress and identify areas for improvement.
- Create Dashboards for Visibility: Display real-time metrics in an easy-to-understand format for your team.
- Monitor Regularly: Review metrics weekly or monthly to ensure continuous improvement.
WWS Value Proposition
At WWS, we empower DME providers with tools to track and analyze critical metrics, including:
- Custom Dashboards: Visualize real-time data and measure performance against benchmarks.
- Automation Solutions: Streamline workflows to improve metrics like claim denial rates and productivity.
- Training and Support: Help your team interpret data insights and turn them into actionable strategies.
Partner with WWS to track the right metrics and unlock your practice’s full potential.



