Answer Summary
AI-driven automation reduces claims denials by enforcing structural reliability across the revenue cycle, transforming intake and documentation into preventative systems that identify inconsistencies before submission. As CMS increases its reliance on automated oversight in 2026, providers utilizing AI-integrated workflows are projected to see a 20% reduction in Days Sales Outstanding (DSO) by eliminating manual documentation gaps. This architectural shift ensures that compliance is built into the workflow, preventing the predictable denials that currently plague reactive billing models.
Introduction: Denials Are a Workflow Failure, Not a Billing Error
For years, claims denials in the DME space were treated as a downstream billing problem. If a claim denied, it moved into a work queue, staff corrected the error, an appeal was filed, and operations moved on. This reactive approach was imperfect but workable when payer reviews relied heavily on human discretion and denial volume remained manageable.
By 2026, that model collapsed.
Payers now rely on automated systems to identify inconsistencies, documentation gaps, and deviations from expected patterns long before a claim reaches a human reviewer. Denials occur faster, at greater scale, and with far less tolerance for inconsistency. In this environment, even experienced billing teams cannot “outwork” structural process flaws.
The reality DME providers must accept is this: most denials are not billing mistakes; they are predictable outcomes of unstable workflows. AI-driven automation does not fix denials by appealing faster—it reduces denials by enforcing reliability across the revenue cycle.
Mapping the DME Revenue Cycle as a Denial Engine
To understand how automation reduces denials, providers must first understand where denials are actually created.
The DME revenue cycle is a chain of dependent stages:
- Intake
- Documentation collection
- Authorization
- Claim submission
- Post-submission feedback
Denials rarely originate at the final step. They are the result of compounding variability introduced earlier—often invisible until submission. An incomplete intake, a weak medical necessity narrative, or an expired authorization may not stop a claim from being submitted, but payer systems will detect the inconsistency immediately.
Traditional operations rely on staff experience to compensate for these gaps. In automated payer environments, that compensation no longer works. Reliability must be built into the workflow itself.
Intake Architecture: Where Most Denials Are Born
Intake is the single highest-risk stage of the DME revenue cycle. It is where payer rules, product complexity, referral quality, and staff judgment collide.
Common intake failures include:
- Inconsistent documentation requirements by payer
- Reliance on memory instead of standardized rules
- Allowing incomplete records to advance “temporarily”
- Treating intake as administrative rather than clinical
AI-driven intake automation addresses these risks by enforcing structure. Instead of relying on staff to remember requirements, systems validate required elements based on payer, product category, and service type. Missing documentation is flagged immediately, and records are prevented from moving downstream until requirements are met.
This approach does not slow operations—it prevents rework. By eliminating variability at intake, providers reduce denial exposure across the entire cycle.
Documentation Integrity as a System, Not a Checklist
One of the most persistent misconceptions in DME billing is that documentation either exists or does not. In reality, most denials occur because documentation is present but insufficient.
A physician order may exist, but the medical necessity narrative may not align with payer expectations. Supporting notes may be included, but not connected clearly to the billed item. These weaknesses are difficult for staff to identify consistently, especially under volume pressure.
AI-driven documentation validation shifts the focus from presence to sufficiency. By comparing current records against patterns from previously approved claims, automation can flag documentation that meets technical requirements but lacks substantive support. This allows providers to strengthen records before submission rather than discovering weaknesses after denial.
Authorization Workflow Automation and Expiration Control
Authorization-related denials increased significantly heading into 2026. Manual tracking methods—spreadsheets, reminders, and staff memory—proved unreliable under volume and staffing constraints.
AI-supported authorization workflows reduce risk by:
- Tracking authorization status in real time
- Monitoring expiration dates automatically
- Validating authorization parameters against payer rules
- Alerting staff before expiration creates exposure
Automation does not eliminate authorization complexity, but it ensures consistency. When authorization controls are embedded into workflows, denials caused by expired or mismatched authorizations decline sharply.
Claim Submission: Moving Beyond Basic Scrubbers
Traditional claim scrubbers focus on formatting and coding errors. While necessary, they are no longer sufficient.
AI-driven claim review introduces risk-based analysis. Instead of asking “Is this claim formatted correctly?” systems ask “Does this claim resemble claims that have historically been denied?”
By analyzing outcomes across payers and product categories, AI can:
- Identify claims that deviate from successful patterns
- Flag submissions requiring human review
- Adjust thresholds dynamically as payer behavior changes
This approach prevents submission of claims that are technically clean but structurally weak.
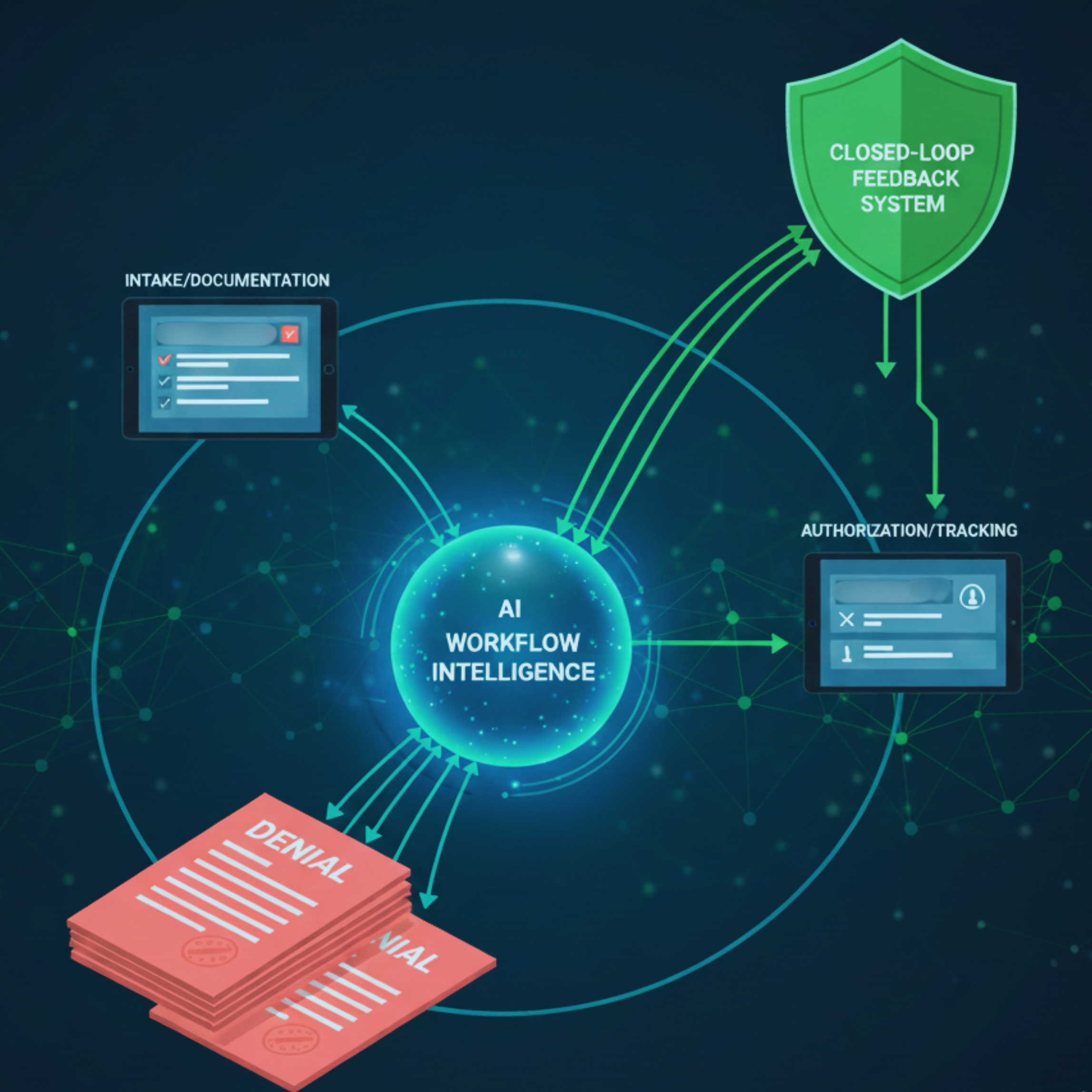
Feedback Loops: Turning Denials Into Workflow Intelligence
Most providers track denials, but few use them effectively. Denial reports often list reasons without connecting them to upstream process failures.
AI enables closed-loop feedback systems by linking denial outcomes back to workflow stages. For example, repeated denials for medical necessity can be traced to specific intake or documentation practices. Authorization denials can reveal gaps in tracking or payer rule interpretation.
By feeding this information back into workflow rules, providers prevent repeat failures. Denials become signals for system correction rather than recurring problems.
Human Oversight and Governance in Automated Workflows
Automation reduces denial risk only when paired with governance. Without oversight, automated systems can scale errors as efficiently as they scale success.
Effective governance defines:
- Which decisions automation can make independently
- When human review is required
- How exceptions are escalated
- How outcomes are monitored and adjusted
Under 42 CFR § 424.57, DMEPOS suppliers remain fully responsible for billing accuracy and documentation integrity, regardless of automation. Governance protects both compliance and operational control.
Measuring Success: Workflow Metrics That Actually Matter
Denial rate alone is an insufficient performance measure. Providers must track metrics aligned to workflow health, including:
- First-pass claim acceptance rates
- Intake fallout rates
- Documentation rework frequency
- Authorization-related denial trends
- Time from service delivery to clean submission
These metrics provide actionable insight into where workflows succeed or fail.
Common Failure Modes When Providers Automate Too Fast
Providers encounter problems when they:
- Automate unstable workflows
- Skip cross-department coordination
- Treat AI as a staffing replacement
- Fail to monitor automated outcomes
Automation amplifies existing process quality. When workflows are inconsistent, automation increases denial exposure rather than reducing it.
Financial Impact of Workflow-Centered Automation
Reducing denials upstream improves:
- Cash flow predictability
- Staff productivity
- Appeal costs
- Audit readiness
The return on automation investment comes from prevention, not recovery. Providers that focus solely on faster appeals miss the larger financial opportunity.
How Wonder Worth Solutions Supports Workflow-Centered Denial Reduction
Wonder Worth Solutions helps DME providers evaluate workflow stability before automation, identify denial drivers tied to process stages, and design governance models that protect compliance while improving efficiency.
The focus is durable improvement, not short-term fixes.
Conclusion: Denial Reduction Is an Architecture Problem
In 2026, claims denials reflect system design more than staff performance. AI-driven automation reduces denial risk when it enforces consistency, strengthens documentation, and closes feedback loops across the revenue cycle. Providers that treat denial reduction as an architectural challenge—rather than a billing task—position themselves for long-term stability.



