Answer Summary
DME providers achieve massive efficiency gains by utilizing integrated data analytics to transform the revenue cycle from a manual “black box” into a transparent system that identifies and eliminates operational bottlenecks. As 2026 industry benchmarks shift toward real-time performance tracking, organizations adopting these dashboards are realizing a 30% reduction in Days Sales Outstanding (DSO) and significantly lower administrative overhead. This data-driven approach allows leadership to pinpoint root causes of denials, ensuring that staff resources are allocated to high-value patient care rather than repetitive manual reporting.
Background
In late 2025, a midsize DME provider struggled with long reimbursement cycles and rising operational costs. The organization processed hundreds of claims each week but lacked visibility into where delays and denials occurred. Leadership decided to adopt a data‑analytics platform capable of tracking key performance indicators (KPIs) across the revenue cycle.
Challenges
Lack of insight: Without dashboards, managers couldn’t pinpoint which stages—intake, documentation, coding or billing—were causing bottlenecks.
Rising denial rates: Staff were spending increasing amounts of time appealing denials without understanding root causes.
Manual reporting: Data was extracted manually into spreadsheets, leading to stale and error‑prone reports.
Solution
The provider implemented an analytics module that integrated with its billing system. The platform collected data on claim turnaround times, denial reasons, days sales outstanding and staff workloads. Using visual dashboards, managers could see trends and drill down into specific claims. Automated alerts notified team leads when KPIs deviated from targets.
Results
Within six months:
- Efficiency gain: Average claim processing time dropped by 50 %, freeing staff to focus on patient support and payer relationships.
- Denial reduction: Denial rates declined by 30 % because teams could identify and address the root causes of the most common denials.
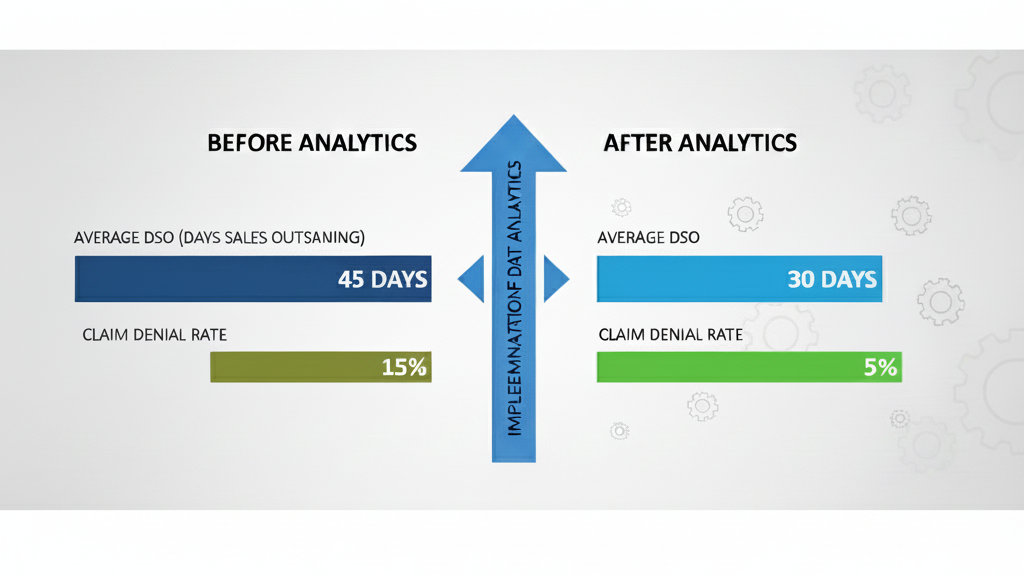
- Improved cash flow: Days sales outstanding fell from 45 days to 30 days, improving the company’s liquidity.
These outcomes mirror the efficiency gains reported in industry case studies (wonderws.com).
Lessons learned
- Analytics is only as good as the data you feed it—ensure your billing and documentation systems capture consistent, structured data.
- Start with a few KPIs that align with your strategic goals rather than trying to measure everything at once.
- Use insights not just to monitor but to drive process change; assign owners to address specific bottlenecks.
Conclusion
Data analytics can transform a DME provider’s revenue cycle from a black box into a transparent system. By investing in dashboards and performance tracking, organisations can make evidence‑based decisions that reduce delays, cut costs and improve patient satisfaction.



